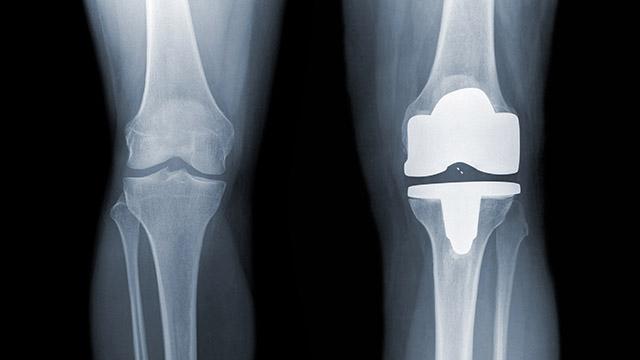
The timing of knee replacement surgery is critical to optimize its benefit. But 90% of patients with knee osteoarthritis who would potentially benefit from knee replacement are waiting too long to have it and getting less benefit. In addition, about 25% of patients who don’t need it are having it prematurely when the benefit is minimal, reports a new Northwestern Medicine study.
This is believed to be the first study to prospectively examine the timeliness of knee replacement among a large number of patients with knee osteoarthritis who could benefit from the surgery. Few prior studies have quantified timeliness of surgery but only among patients who already had knee replacement, and these studies generally were in smaller cohorts of patients.
“People are waiting and waiting to have the procedure and losing the most benefit,” said lead investigator Hassan Ghomrawi, associate professor of surgery at Northwestern University Feinberg School of Medicine.
African-Americans delayed knee replacement surgery more than Caucasians, the study found.
“When people wait too long, two things happen,” Ghomrawi said. “The osteoarthritis causes deterioration of their function. Some of them wouldn’t be able to straighten out their legs, affecting their walking and mobility. When you can’t get exercise, you can start to develop other health problems such as cardiovascular problems. You may also become depressed. The overall impact can be huge.”
The second problem with delaying surgery is less benefit. “You don’t get as much function back when you wait too long; your mobility is still reduced versus somebody who had it in a timely fashion,” Ghomrawi said.
The ideal timing of knee replacement surgery is based on an algorithm that factors in pain, joint function, radiographic assessment and age to determine if a person will benefit from surgery.
Getting knee replacement surgery too early based on the algorithm means patients are having major surgery with risk of complications and getting minimal benefit. They may also need a revision (second surgery) later in life, which is a much more difficult surgery with poorer outcomes than the original surgery.
The study was published Jan. 13 in the Journal of Bone and Joint Surgery.
Nearly 1 million knee replacement procedures are performed in the U.S. each year with projections of a rapid increase by 2030, the paper reports.
“As the number of surgeries rises, we need to make sure the timing is optimal for patients to obtain the most benefit and to keep health care costs down,” Ghomrawi said. “Because knee replacement is an elective procedure, the timing of surgery is susceptible to not just clinical factors but also demographic, socioeconomic and sociocultural ones. We need to develop a better understanding of these factors to improve timing of surgery.”
The Northwestern study was based on 8,002 participants who had or were at risk for knee osteoarthritis and were followed for up to eight years as part of two diverse multicenter trials, the Osteoarthritis Initiative and Multicenter Osteoarthritis.
Dr. Leena Sharma of Northwestern is a study coauthor.
The study was funded by grants R21-AR069867 and P30-AR072579 from the National Institute of Arthritis and Musculoskeletal and Skin Diseases of the National Institutes of Health.