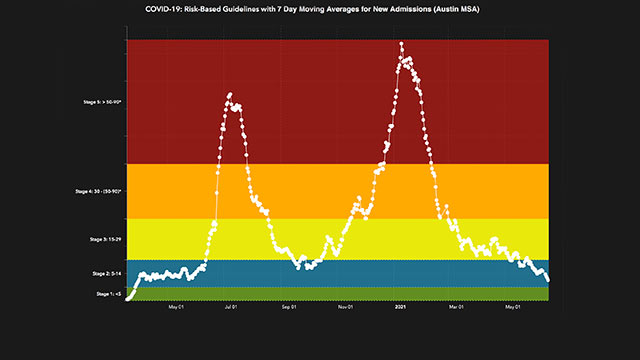
In a new study led by The University of Texas at Austin COVID-19 Modeling Consortium in collaboration with Northwestern University, researchers describe the alert system that has guided COVID-19 policies in Austin, Texas, for more than a year, helping to safeguard the health care system and avoid costly measures. The system tracks the number of new daily COVID-19 hospital admissions and triggers changes in guidance when admissions cross specific threshold values. While using this staged alert system, the Austin metropolitan area has sustained the lowest per capita COVID-19 death rate among all large Texas cities.
“Austin’s alert system was optimized to balance the city’s public health and socioeconomic goals,” said Lauren Ancel Meyers, a professor of integrative biology and director of The University of Texas COVID-19 Modeling Consortium. “For over a year, it has helped our community adapt to rapidly changing risks, protected the integrity of our hospital systems and limited the economic damage.”
The study was published today (June 18) in the journal Nature Communications.
Throughout the COVID-19 pandemic, policymakers struggled to combat COVID-19 while minimizing social and economic consequences. Governments worldwide enacted a variety of alert systems that trigger lockdowns when cases or hospitalizations reach critical levels. According to the paper, Austin’s system was better at preventing overwhelming hospital surges than the ICU-based triggers used in France and better at avoiding lockdowns than widely cited recommendations from Harvard Global Health.
"Our flexible method can design adaptive policies to combat COVID-19 worldwide and prepare for future pandemic threats,” Meyers said. “When we compared Austin’s optimized triggers to other similar alert systems, we found that it does a much better job of balancing competing public health and economic goals.”

Northwestern’s David Morton designed the study with Meyers and Haoxiang Yang, a postdoctoral research associate at the Center for Nonlinear Studies (CNLS) at Los Alamos National Lab.
"The success of Austin’s system stems partly from its reliance on hospital admission data, which provides a more reliable signal of COVID-19 transmission than reported cases, and partly from our rigorous optimization of the alert triggers," Morton said. The researchers derived thresholds that provided a 95% guarantee that hospitals would not be overrun.
Morton is the David A. and Karen Richards Sachs Professor of Industrial Engineering and Management Sciences at the McCormick School of Engineering. He also is chair of the department.
The three Austin-area hospital systems, Ascension Seton, St. David's HealthCare and Baylor Scott & White Health, provided key data that were not available in most other U.S. cities in the early months of the pandemic, including estimates for ICU and hospital capacity and daily reports of new COVID-19 hospital admissions.
This work was supported by the National Institutes of Health, the Texas Department of Human Services, the Centers for Disease Control and Prevention, CNSL, the Bavarian-Czech Academic Agency, Tito’s Handmade Vodka and the Texas Advanced Computing Center at The University of Texas at Austin. Meyers holds the Denton A. Cooley Centennial Professorship at The University of Texas at Austin.