CHICAGO - Having to strip down regularly to have your partner check for mole irregularities may be initially embarrassing to a person -- especially a woman -- previously diagnosed with melanoma.
But a new Northwestern Medicine study shows the benefits of a partner frequently checking for troublesome moles based on training to do so far outweigh the embarrassment.
When the trust is there (between partners), there’s no issue with embarrassment.”
Lead and senior author, research professor of dermatology at Northwestern University Feinberg School of Medicine
Study participants who received skin examination training caught far more mole irregularities than those in the control group. They also grew more confident performing the examinations.
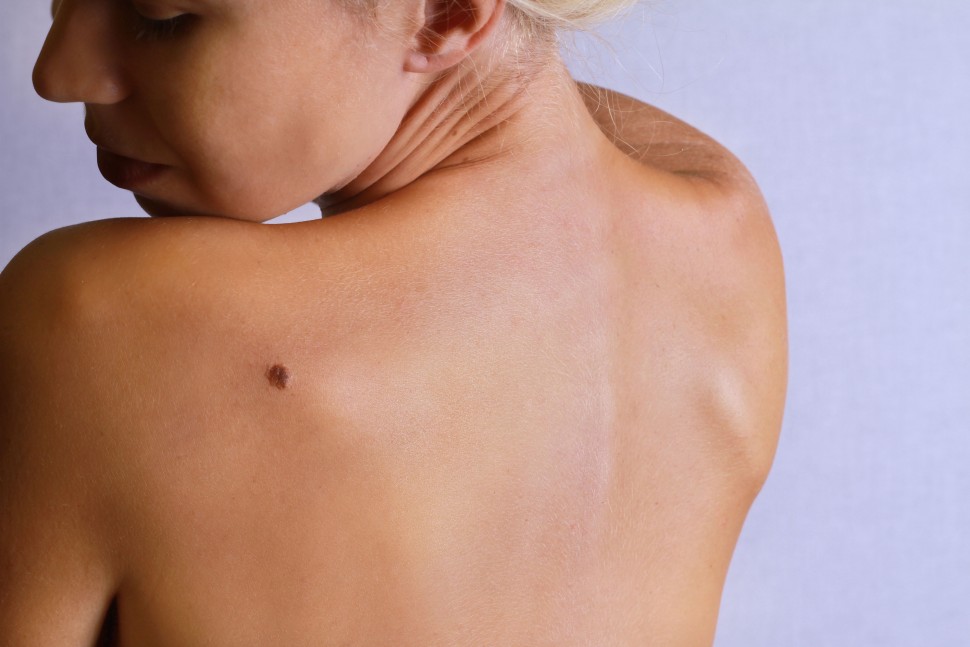
Common places to develop potentially fatal melanoma include hard-to-see areas where it is difficult to apply sunscreen such as behind the ears and knees, the top of the head and around the swimsuit line on a woman’s bottom.
“These aren’t parts of the body that most females like to have examined by their male partner, but at some point, they realized they’re just looking at the moles, not the cellulite,” said lead and senior author Dr. June Robinson, research professor of dermatology at Northwestern University Feinberg School of Medicine. “We found as long as the benefit is strong enough, it overcomes whatever potential embarrassment there might be between the partners.”
Partners of patients who had been previously diagnosed with early stages of melanoma performed frequent skin self-self examinations (SSEs) on the patient over the course of the two-year study.
As the study progressed, a partners’ confidence in his or her ability to find irregular moles increased, as did the trust in one another to successfully identify the irregularities.
The study was published today (Dec. 14) in JAMA Dermatology.
Partners examined hard-to-see areas such as the top of the head and the back of the knees and ears, which are common places to develop fatal melanoma
Participants were asked every four months to indicate on a five-point scale how much they agreed or disagreed with the following two statements: “It is very embarrassing to have my partner help examine my skin,” and “I am very comfortable having my partner help examine my skin.”
Based on their responses, melanoma patients and their partners eventually had no problems being checked for irregular moles by their partners, Robinson said.
“In that discussion back and forth, they make a judgment call and agree on it,” said Robinson, who is the editor of JAMA Dermatology and a member of the Robert H. Lurie Comprehensive Cancer Center of Northwestern University. “As they each grow more confident in their decision-making, the trust between them becomes stronger. When the trust is there, there’s no issue with embarrassment.”
Also noteworthy, the study found mole observations men and women make complement one another. Men tend to notice mole border irregularities better than women, whereas women tend to see color variations in the moles better than men.
“The pairs realize, ‘We need to help each other here,’” Robinson said. “If he sees borders better and she sees colors better, those two heads are better than one when finding the irregularities.”
Men observe mole border irregularity better than women, who notice color variations better
The 395 participants in the study had previously been diagnosed with early stages of melanoma (0 to IIB) and had surgically removed irregular moles. They were recruited from outpatient clinics of the Northwestern Medicine and were 21 to 80 years old.
The control group consisted of 99 participants who did not receive SSE training. The remaining participants received training in one of three forms: from a physician, by reading a take-home handbook or by listening to exercises on a tablet. The pairs performed SSEs on one another every month or every other month to check for mole irregularities, and assigned a score to common features of the mole: 1 if the mole looked normal, 2 if they were unsure and 3 if it looked abnormal.
Robinson’s study received a four-year renewal, allowing her to continue following the participants and checking in every four months on their progress and levels of embarrassment, comfort and confidence with partner-assisted SSEs.
The study was supported by grant R01 CA154908 from the National Cancer Institute of the National Institutes of Health.